No. 14: First Aid-Theory, basics, demonstration, hands on training, audio-visuals and practice, BLS systems. – SCA
Aim:
To demonstrate the first aid- Basic Life Support (BLS) for sudden cardiac arrest and prepare a poster or leaflet about Cardiopulmonary resuscitation (CPR).
Practical Significance:
Sudden cardiac arrest (SCA) is a primary cause of death that can strike anyone at any age. Pharmacists must create awareness in society about the first aid measures to be taken if someone suffers from SCA. In this practical session, students will learn about the steps to perform cardiopulmonary resuscitation (CPR) and operate an automated external defibrillator (AED) so that they can educate society about these procedures.
Theory:
Sudden cardiac arrest (SCA) is a condition in which the heart stops beating suddenly and unexpectedly. Blood flow to the brain and other essential organs is cut off as a result. SCA usually results in death if not addressed within minutes.
The heart has a self-regulating electrical mechanism that ensures proper heart function. The pacemaker cell (SA node) and latent pacemaker (AV node, bundle of his) send out a signal that causes electrical activity, which regulates the rate and rhythm of the heartbeat. Problems with the electrical system of the heart can lead to irregular heartbeats and arrhythmia. SCA is caused by certain arrhythmias which cause the heart to stop pumping blood to the body.
SCA is not the same as a heart attack. When blood supply to a segment of the heart muscle is blocked, a heart attack ensues. Usually during a heart attack, the heart does not stop beating suddenly. SCA, on the other hand, can occur after or during the recovery from a heart attack.
SCA is more common in people with heart disease (ventricular fibrillation, ischemic heart disease, coronary artery disease, significant physical stress, certain hereditary abnormalities, and anatomical alterations in the heart). SCA can, however, occur in persons who appear to be healthy and have no documented cardiac disease or other risk factors.
Symptoms of SCA
- Loss of consciousness (be unresponsive) b) No breathing (be not breathing normally)
- No pulse
- No movement or signs of life.
- Before fainting, some people experience a racing heart, dizziness, or light-headedness. Some people experience chest pain, shortness of breath, nausea (feeling sick to the stomach), or vomiting an hour before SCA.
First Aid in SCA
Sudden cardiac arrest is a life-threatening situation. A person with SCA should be treated with a defibrillator as soon as possible. An electric shock is delivered to the heart using this device. An electric shock can help a heart that has stopped beating regain its regular rhythm. Defibrillation must be performed within minutes after SCA for it to be effective. The chances of surviving SCA gradually decrease with each passing minute. One must immediately call the medical emergency service if he/she finds a person suffering from SCA. A person with SCA should receive cardiopulmonary resuscitation (CPR) until defibrillation can be performed.
Cardio-Pulmonary Resuscitation (CPR)
CPR is a life-saving procedure performed when a person’s breathing or heartbeat has stopped. This could happen because of a medical emergency, such as an electric shock, a heart attack, or drowning. CPR is a technique that combines rescue breathing with chest compressions. Rescue breathing supplies oxygen to the person’s lungs. Chest compressions keep oxygen-rich blood moving until the heartbeat and breathing can be restored.
Steps before performing CPR
- First and foremost, assess the situation and the individual. Once the scenario is safe, tap the person on the shoulder and ask, “Are you OK?” to see whether the person requires assistance.
- If it’s clear that the person needs assistance, call medical emergency (or ask someone nearby to call), and send someone to get an automated external defibrillator (AED).
- Make sure the airway is clear. Tilt the head back slightly to elevate the chin while the person is lying on his or her back.
- Check whether the person is breathing. Listen for sounds of breathing for no longer than 10 seconds. (Gasping sounds are not the same as breathing.) Start CPR if the person is not breathing.

Checking whether person requires assistance
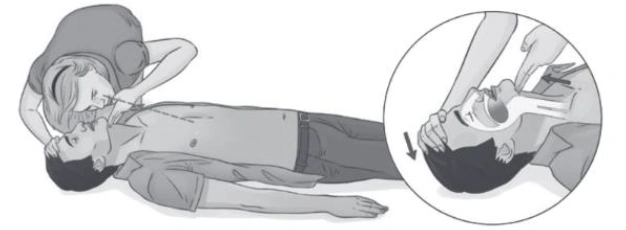
Checking whether person is breathing
Steps to be followed for CPR (As per National Health Portal)
A. Compression
- Place the heel of one hand on the lower half of the person’s breastbone.
- Place the other hand on top of the first hand and interlock your fingers.
- Press down firmly and smoothly (compressing to 5-6 cm) 30 times.
- Administer 2 breaths as described below in mouth-to-mouth.
- The ratio of 30 chest compressions followed by 2 breaths is the same, whether CPR is being performed alone or with the assistance of a second person.
- Aim for a compression rate of 100 to 120 per minute.
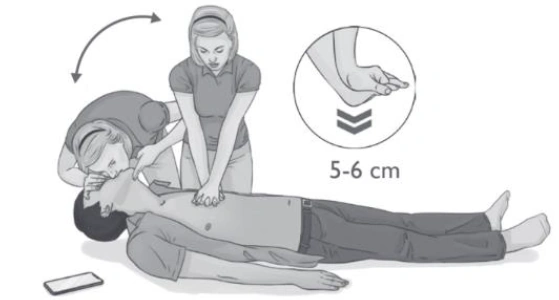
Compression followed by mouth-to-mouth respiration
B. Mouth-to-mouth respiration
- If the patient is not breathing normally, make sure he is lying on his back on a firm surface.
- Open the airway by tilting the head back and lifting his chin.
- Close his nostrils with your finger and thumb.
- Put your mouth over the patient’s mouth and blow into his mouth.
- Give two full breaths to the patient (this is called ‘rescue breathing’). Make sure there is no air leak and the chest is rising and falling. If patient’s chest does not rise and fall, check that you’re pinching his/her nostrils tightly and sealing his/her mouth with your mouth. If still no breathing, check airway again for any obstruction.
- Continue CPR, repeating the cycle of 30 compressions followed by two breaths until availability of AED or arrival of medical help.
Usually, CPR should be stopped, when:
- The patient revives and starts breathing on his/her own.
- When medical help arrives.
- When the person giving CPR is exhausted.
Points to remember during CPR:
- Maintain as much straightness in your arms as possible. Arm muscles fatigue faster than your body weight. Maintaining adequate depth by keeping the arms straight helps the body weight drive the compression down.
- During compressions, keep your hands continuously in touch with the person’s chest.
- The shoulders of the person given CPR should be up over the person. This position guarantees that compressions are directed downward and that the heart is compressed between the sternum and the spine.
- The hands must be straight over each other to increase the compression force.
- Interlace the fingers or place one hand on top of the other with fingers extended away from the patient’s chest.
- Full recoil of the chest is as important as the depth and rate of chest compressions.
- Without proper depth (at least 2 inches), compressions are not effective.
Result:
The first aid- Basic Life Support (BLS) -CPR for sudden cardiac arrest was demonstrated.
